Chronic diseases are going to skyrocket, straining the nation’s healthcare system.
Longer American lifespans coupled with younger generations who are not taking care of themselves are cause for concern. If changes are not made soon, the burden on healthcare providers, patients and the entire system will grow.
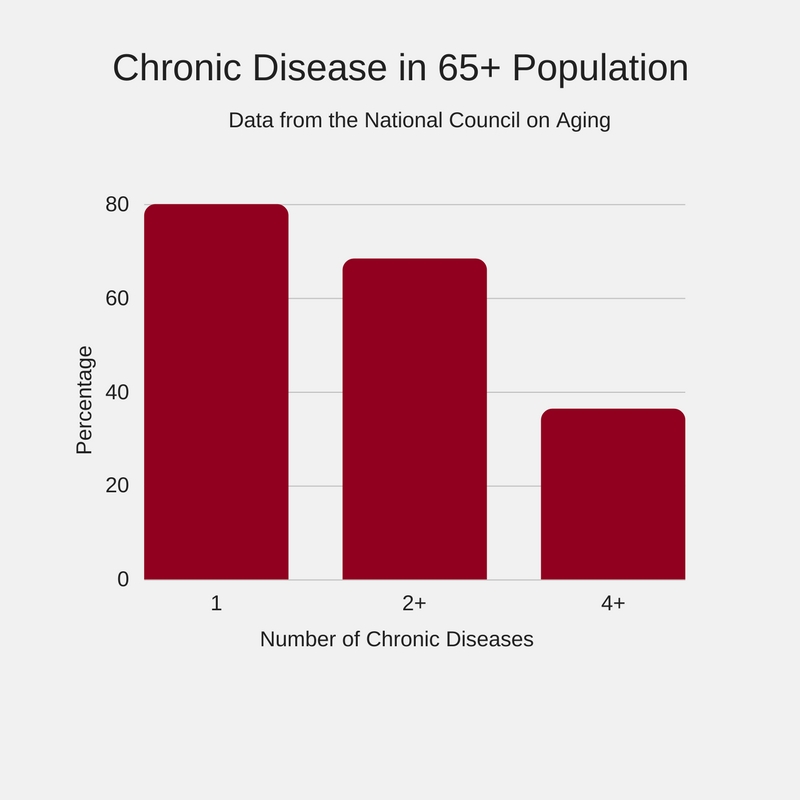
As of 2012, nearly half of all adults – 117 million people – lived with one or more chronic disease or condition, according to the most recent data available from the Centers for Disease Control (CDC). One in four had two or more conditions. According to the National Council on Aging (NCOA), that percentage increases in older adults.
Rates within the older population will rise. In 2015, 15% of the population, about 47 million people, were 65 or older.
What is a Chronic Disease or Condition?
While there are slight variations in the definition of “chronic disease” or “chronic condition” within the medical, policy and academic communities, as explained in a 2016 report published by Frontiers in Public Health, the terms commonly refer to physical or mental health conditions or diseases that have long-lasting effects that require ongoing medical attention.
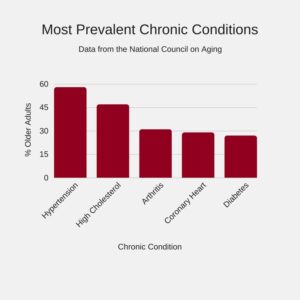
The Centers for Medicare and Medicaid Services lists 19 chronic disease and conditions, including Alzheimer’s disease, Depression, Hyperlipidemia (high cholesterol) and Hypertension (high blood pressure).
Chronic Disease and Conditions Affect Healthcare Spending
People living with a chronic disease or condition use more healthcare services and account for higher spending than those who are healthy. About 71% of total healthcare spending is associated with adults living with chronic diseases or conditions, with spending significantly increasing for those living with multiple diagnoses.
According to the 2017 report “Multiple Chronic Conditions in the United States,” all adults who have five or more chronic conditions account for 41% of healthcare spending, which includes office visits, inpatient visits and prescriptions. The report also reveals they use twice as many drugs each year, compared to people with three or four conditions. Additionally, adults with five or more conditions average 20 doctor visits per year, compared to 12 visits for those with three or four conditions.
Prevention and Treatment: A Working Solution
How can people, providers and organizations bend the trajectory of chronic disease and its impact on the healthcare system?
New treatment models, prediction tools and community programs aimed at improving overall health are being tested and developed to improve detection, prevention and management of chronic diseases and conditions.
Prevention Efforts
Many chronic diseases and conditions including heart disease, diabetes and obesity are preventable. Lack of physical activity, poor diet, and tobacco and alcohol use contribute to poor health and increase risk factors.
To increase awareness and promote a healthy lifestyle, the CDC is continuously partnering with local and national public health organizations to maintain and launch new chronic disease prevention programs. Information about individual state programs can be found on the CDC’s State Snapshots tool.
Additionally, medical breakthroughs are helping medical providers improve risk detection. Imagine a blood test that can predict – within three years – your risk of developing a chronic disease?
According to a 2017 article published by National Public Radio, researchers with the Intermountain Medical Center Heart Institute in Salt Lake City developed a blood test that was proven to be 77-78% accurate in predicting diabetes, coronary artery disease, dementia and other illnesses. Having better knowledge about risk can better help people make necessary health changes now, before a potential diagnosis.
Treatment Options
The healthcare system is largely designed to treat individual problems rather than the person as a whole. Major changes need to take place to address fragmented care, according to Stanford University School of Medicine Professor Kate Lorig.
“Right now, (the system) addresses diseases or even parts of diseases or small sub-parts of the body. It does not address the whole, complex person with multiple chronic diseases. So, right now what happens, if you’re lucky, you go to a primary care doc who kind of does the day-to-day stuff and then you see four or five specialists each of which do their little specialty part – none of whom really talk to each other except maybe to look at your laboratory tests on an electronic medical record if you’re really lucky,” Lorig explains in an interview with Kaiser Health News.
However, creating an integrated care model and proving success can be achieved.
According to a 2014 article in the Harvard Business Review, the Virginia Mason Health System deployed integrated multi-specialty care models for conditions such as headaches, joint pain and chest pain, and when done so in conjunction with major employers in Seattle, organizations witnessed health-related absenteeism drop by 50%.
Until treatment challenges are addressed nationwide, there are other ways healthcare providers and organizations can help patients. For example, Self-management programs offered through the National Council on Aging and Stanford University’s Self-Management Resource Center.
The Chronic Disease Self-Management Program offered through Stanford University features workshops – held in senior centers, churches and hospitals – that help people cope with the effects of living with a chronic disease, including topics around communication, nutrition and exercise and knowledge of medication regimes.